May 5, 2026
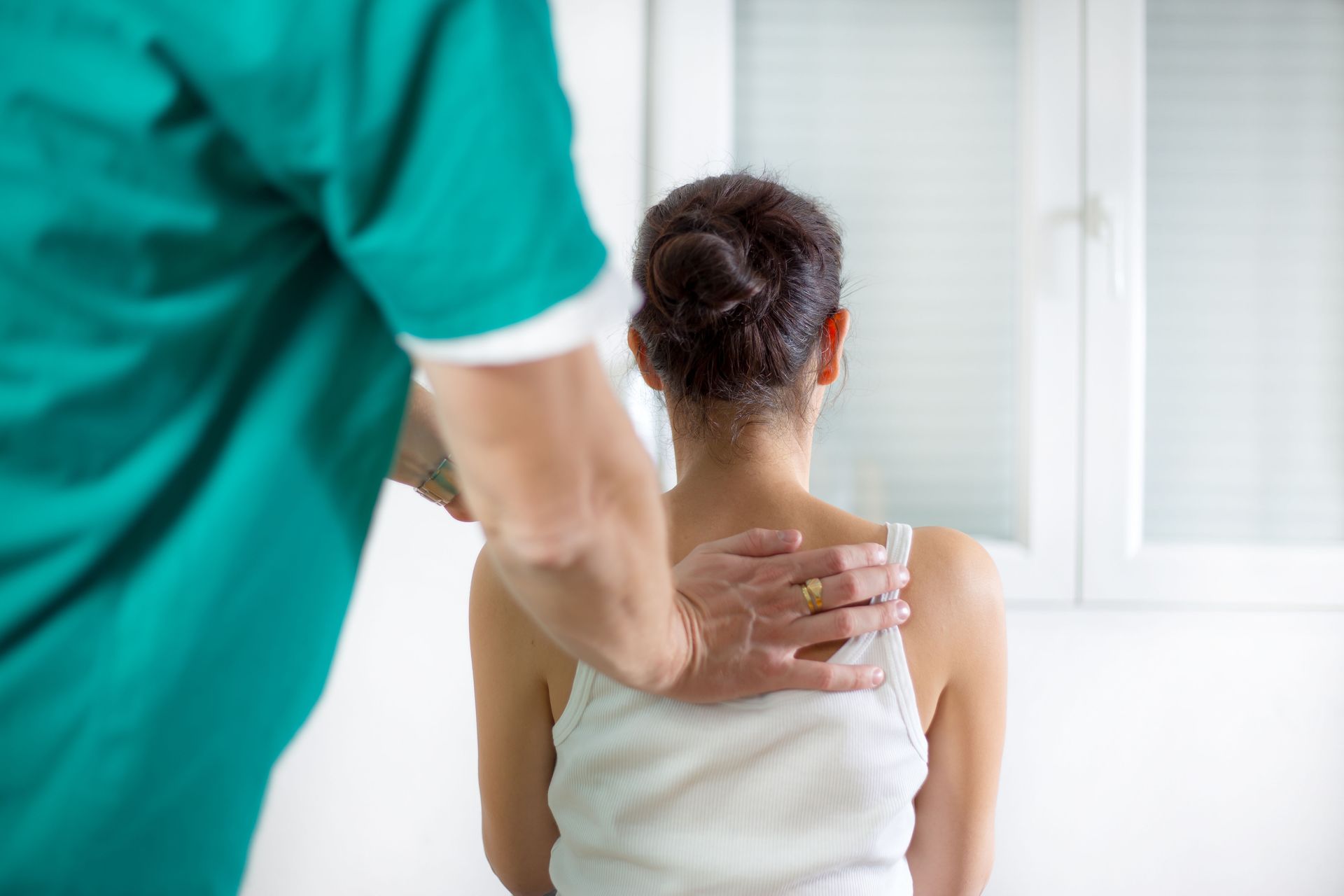
Navigating the journey toward recovery after a significant health event or chronic diagnosis often feels like walking through dense fog. The path is rarely linear, and the physical limitations that arise can impact every facet of daily existence. From the simple act of rising from a chair to the complex movements required for professional athletics, our mobility defines our independence. When the body fails to cooperate due to injury or illness, the intervention of specialized clinical care becomes the bridge between disability and a return to form. This specialized care, often referred to as physical rehab, focuses on restoring function, improving strength, and teaching the body how to compensate for permanent changes while maximizing remaining potential.
As the global understanding of preventative and restorative care evolves, more individuals are seeking out professional assistance to manage their physical well-being. This shift is reflected in the massive scale of the professional landscape. According to Towards Healthcare, the physical therapy industry is expected to grow from $28.06 billion in 2024 to $41.54 billion by 2034. This growth underscores the essential nature of rehabilitative services in modern society, particularly as populations age and the desire to maintain an active lifestyle remains a top priority for people across all demographics.
1. Neurological Disorders and Stroke Recovery
Neurological conditions represent some of the most challenging hurdles for any individual, as they affect the communication lines between the brain and the limbs. When a stroke occurs or when a patient manages a condition like multiple sclerosis or Parkinson’s disease, the primary goal of physical rehab is to exploit the concept of neuroplasticity. This is the brain’s ability to reorganize itself by forming new neural connections throughout life. By engaging in repetitive, purposeful movements, patients can essentially "teach" healthy parts of the brain to take over functions previously managed by damaged areas.
The recovery process for neurological patients is often intensive and requires a high level of patience. It involves a variety of techniques designed to improve balance, coordination, and gait. For instance, a person who has lost sensation or control on one side of their body must relearn how to distribute their weight evenly to prevent falls. The structured environment of a clinical setting provides the safety and specialized equipment—such as parallel bars or body-weight-supported treadmill training—necessary to practice these skills without the risk of injury.
Specific benefits for neurological patients include:
- Enhancement of motor control and fine motor skills.
- Reduction in muscle spasticity and painful cramping.
- Improvement in vestibular function to decrease dizziness.
- Development of compensatory strategies for sensory loss.
2. Orthopedic Injuries and Post-Surgical Healing
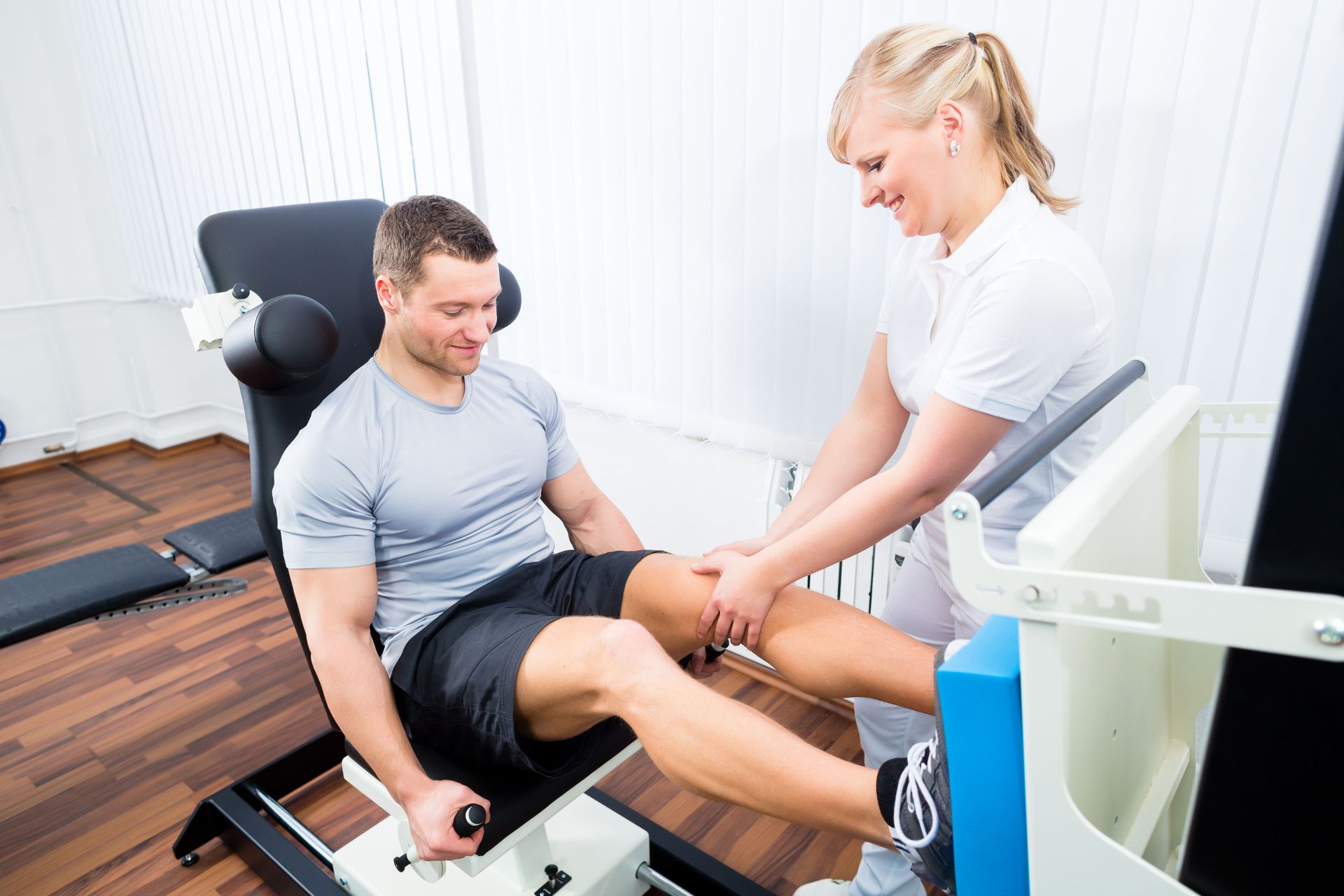
Orthopedic conditions constitute the most common reasons individuals seek out professional help. The skeletal system and its supporting soft tissues are prone to wear and tear over time, as well as acute damage during physical activity. When a person undergoes a procedure like a total knee replacement or a rotator cuff repair, the surgery is only the first step. The true work begins in the weeks following the operation, where physical rehab is utilized to ensure the joint does not freeze up or become encased in excessive scar tissue.
In the aftermath of an orthopedic surgery, the body’s natural response is to protect the area by inducing inflammation and guarding the muscles. While this is helpful in the initial days, prolonged guarding leads to weakness and a loss of flexibility. Clinicians work with patients to gently break through these barriers. They use manual therapy techniques and guided resistance training to manage pain while pushing the boundaries of what the limb can do.
Common orthopedic goals involve:
- Restoration of full range of motion in the affected joint.
- Strengthening of postural muscles to alleviate pressure.
- Education on proper body mechanics to prevent re-injury.
- Optimization of performance for those returning to sports.
3. Cardiac Events and Pulmonary Endurance
Cardiovascular and pulmonary health are vital components of physical rehab that are often overlooked by the general public. After a heart attack, heart surgery, or the onset of chronic obstructive pulmonary disease, the body becomes deconditioned. The heart is a muscle, and like any other muscle, it requires specific training to regain its efficiency. These programs provide a monitored environment where patients can increase their heart rate safely under clinical supervision.
The focus here is on increasing aerobic capacity and teaching the patient how to manage shortness of breath. Through progressive exercise, the circulatory system becomes more adept at delivering oxygen to the tissues, which reduces the overall strain on the heart. This type of intervention is life-saving, as it significantly lowers the risk of future cardiac events and improves the patient’s ability to perform daily chores without exhaustion.
4. Chronic Pain and Spinal Misalignment
Persistent pain in the lower back, neck, or joints can be debilitating, often leading to a cycle of inactivity and further discomfort. Many patients turn to physical rehab as a non-invasive alternative to surgery or long-term medication use. By identifying the root cause of the pain—which is often a combination of muscle imbalances, poor posture, and joint stiffness—clinicians can create a targeted plan to realign the body and reduce the load on sensitive structures.
Stabilization exercises for the core and spine are central to this process. When the deep muscles of the torso are strong, they act as a natural corset, protecting the vertebrae and discs from excessive pressure. This approach not only provides relief from current pain but also equips the patient with the tools to manage flare-ups independently. Learning how to move correctly during lifting, sitting, and sleeping is a core component of this educational journey.
5. Pediatric Development and Congenital Challenges
Children who face developmental delays or were born with congenital conditions such as cerebral palsy or muscular dystrophy benefit immensely from early intervention. In a pediatric setting, physical rehab looks quite different than it does for adults; it often incorporates play-based activities to keep the child engaged while working on fundamental motor milestones. The goal is to help children reach their maximum potential for independence as they grow.
Clinicians work closely with families to integrate therapeutic movements into the child's daily routine. This might include working on head control, crawling, or the transition from sitting to standing. By addressing these needs during the formative years, therapists can help prevent secondary skeletal deformities and ensure that the child has the best possible foundation for physical interaction with the world around them.
6. Geriatric Mobility and Fall Prevention
As the body ages, maintaining balance and bone density becomes a primary concern. For the elderly, a single fall can lead to a catastrophic loss of independence. Geriatric physical rehab focuses on proactive measures to keep seniors on their feet. This includes balance training, strength building to combat age-related muscle loss, and environmental assessments to make the home safer.
Improving proprioception—the body's ability to sense its position in space—is a major focus for older adults. By practicing movements that challenge their equilibrium in a controlled setting, seniors can react more quickly to trips or uneven surfaces in their everyday environment.
Key elements of geriatric care:
- Balance exercises to reduce the frequency of falls.
- Weight-bearing activities to support bone health.
- Flexibility routines to maintain ease of movement.
- Gait training to ensure a steady walking pattern.
Recovering from these conditions is a journey that requires professional guidance, personal dedication, and a clear roadmap for the future. Whether you are dealing with the complexities of a neurological diagnosis or the standard recovery path of a joint surgery, the right support makes all the difference in your quality of life. If you are ready to take the first step toward a more mobile and pain-free living, reach out to the experts at Physical Restoration & Sports Medicine.